
The price you pay is all a black box………………………..
The Feds just asked a huge healthcare company who their real clients are and the answer is totally unsatisfying
Dec. 7, 2017, 4:09 PM
The SEC forced pharmacy benefit manager Express Scripts to break out a seemingly benign number from its balance sheet. It has to do with the rebates it collects from pharmaceutical firms.
- Experts say it’s weird that the company wasn’t breaking this out before.
- The number does, however, speak to a lot of concerns people have about PBMs in general, and who they’re actually serving — their clients or big pharma.
The SEC has been trying to get to the bottom of a very important question for Express Scripts, the country’s biggest pharmacy benefits manager (PBM).
The question is: Who are your clients?
Ideally, in Express Scripts’ business, the client is ultimately you — or whoever pays for your health insurance. The company manages lists called formularies that determine what your insurer will and will not pay for. It’s like a gatekeeper, and it’s the biggest gatekeeper in the country. It, along with PBMs run by CVS and UnitedHealth control 80% of all covered lives in the US.
It is paid by insurers and employers to do this, and the point is to keep costs down — to get you the best medication as cheaply as possible and take on the complicated process of choosing what drugs are worth paying for.
Part of how PBMs do this is by setting up rebates with drug companies. The PBM keeps a portion of it, and passes the rest on to you.
But all of the details of that are top secret. That is to say, why you pay the price you pay is all a black box.
Some people are starting to have a problem with that.
Over the last year or so Washington has been wondering if enough of those rebates are actually being passed along to you. It’s also wondering if those rebates incentivize PBMs to choose expensive drugs that have higher rebates.
Back in June, for example, Senator Bill Cassidy (R-LA) asked experts on a drug pricing panel if rebates “are actually a benefit to our society” since because of them “you may be paying more because you’re on insurance than you would without it.”
There’s also concern that rebates are blocking out the competition. In a recent presentation, the Federal Trade Commission highlighted a lawsuit between Sanofi and Mylan (yes, of EpiPen price gouging fame). Sanofi sued Mylan for offering PBMs and others such fat rebates that it couldn’t sell its EpiPen competitor, Auvi-Q.
It’s not just the government that’s bothered by all this. In fact, Express Scripts’ biggest customer, Anthem Insurance, just dropped it citing sky-high prices for drugs and operational failures.
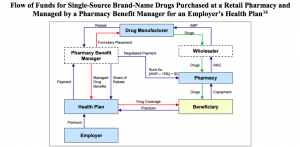
This is how your drugs get to you. The PBM gets to see all of it, you see almost none. American Health Policy
What makes a client?
And a few months ago, the SEC asked Express Scripts why it wasn’t breaking out the rebate money it was getting from pharmaceutical firms on its balance sheet. All of the letters were made public, and you can read them here.
Instead of breaking it out, Express Scripts was just lumping its receivables from pharmaceuticals firms in with receivables from its clients. The SEC wasn’t having that.
From a letter on October 12, 2017 [emphasis ours]:
Rule 5-02.3 of Regulation S-X requires separate disclosure of receivables from customers (trade) and others. It is unclear why you believe accounts receivable from pharmaceutical manufacturers are a component of customer receivables considering that pharmaceutical manufacturers do not appear to be your customer. Please revise your disclosure to separately state accounts receivable from pharmaceutical manufacturers or further explain why you do not believe this is required.
The numbers Express Scripts ended up disclosing are no small thing. At the end of last December pharma receivables — that is, payments due to the company — were $2.2 billion, out of a total $7 billion. By the end of September 2017, pharma receivables were $2.5 billion out of $6.8 billion in total receivables.
We should note that Express Scripts asked for its exchange with the SEC to be made confidential.
Ed Ketz, an accounting professor at Penn State, thought that was odd. He thought it was even odder that Express Scripts wouldn’t disclose its gross rebate receivables.
“I’m amazed that they would balk at this. Just make the disclosure and be done with it… They must have thought this was really important.” he told me.
So what to make of the disclosure?
“I think at 40% [of receivables] we can start thinking of the pharmaceutical companies as customers. They’re not just bystanders in this equation,” he said.
Either way, Ketz told me, disclosing gross rebate receivables would give investors a better understanding of Express Scripts’ business.
“It would clearly be better for investors if we had a better picture of the amounts of rebates.”
Why so secret?
As it stands now, it’s basically impossible to know how much Express Scripts is making from rebates. The company told me that “the bulk” of what it collects from pharma is in rebates, though it does sell some services to drug manufacturers.
It’s also impossible to figure out how much of its rebates get passed along to customers. The company claims that it hands 89% of rebates back to customers, but there are a couple of reasons why that’s hard to figure out from its financial statements, or if you’re a customer.
- As the SEC noted in its letters, Express Scripts gives clients qualitative reasons for its pricing, instead of quantitatively showing clients how rebates lower costs. The company says that quantifying rebates “would be misleading to investors because it is only one of several measures of pricing in any given contract.”
- We don’t know, as Professor Ketz pointed out, how much Express Scripts is collecting in gross rebates. Its insistence on secrecy made him “mostly confused.”
- We don’t know how much non-rebate revenue Express Scripts is getting from pharma. If it’s a significant amount, that tilts the incentive structure in this business toward pleasing pharma. And that’s probably a big conflict for the insurers who pay it huge sums to help them manage costs.
Express Scripts said that its clients can audit the company at any time. But that’s arduous, expensive process for many businesses. Either way, that’s very far removed from what’s really worrying Americans — rising healthcare costs gobbling up more and more of their paychecks.
If it feels like that money is just falling into a black hole, that’s because it is.
SEE ALSO: The big loser in the CVS-Aetna deal already seems pretty clear
_____________________________________
THIS ARTICLE CONTRIBUTED BY:
Brian Klepper, PhD
Principal, Worksite Health Advisors
904.343.2921, bklepper@worksitehealthadvisors.com
Recent Articles
High Performance Health Innovators Could Improve Outcomes, Lower Costs, EBN, 11/06/17
Why Most Health Plans Strive to Make Health Care Cost More, EBN, 8/01/17
How an Indian-Born Caribbean Hospital Could Influence US Healthcare, TDWI, 5/03/17
How Employers Can Get The Most Out of Worksite Clinics, EBN, 4/28/17
How Health City Cayman Islands Innovates, THCB, 4/05/17
The Gold Standard for Current Cancer Treatment, JAMA, 6/26/16

