By Bill Rusteberg
A CPO (Cash Pay Option) centric health plan removes all financial barriers to health care while saving money at the same time. Cash beats insurance everytime.
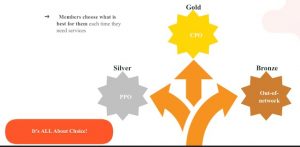
Under this health plan strategy members have the ability to choose the Gold, Silver or Bronze Plan at the point of service.
GOLD PLAN
CPO – Cash Pay Option. Plan pays cash to medical caregivers through plan assets. All patient financial responsibility is waived. Savings average 40% over traditional managed care plans. 75% of plan members will choose this benefit path at the time of service.
SILVER PLAN
PPO – Traditional status quo benefit plan with deductible, copays and coinsurance. 20% of plan members will choose this benefit path at the time of service.
BRONZE PLAN
TPO (Terrible Punishment Option better known as Out-of-Network) – “Nightmare City” with deductible, copays, coinsurance and balance billing. 5% of plan members will choose this benefit path whether they know it or not.
IT’S ALL ABOUT CHOICE
At the point of service plan members have the freedom to determine which benefit plan is best for their individual needs.
CASH IS KING
This CPO centric program is expected to generate savings similar to Reference Based Pricing (RBP) plans but without all the noise and disruption common with moving to RBP. CFO’s and HR have shared enthusiasm embracing this common sense risk management strategy.
“Once we rid ourselves of traditional thinking we can get on with creating the future” – James Bertrand
RiskManagers.us is a specialty company in the benefits market that, while not an insurance company, works directly with health entities, medical providers, and businesses to identify and develop cost effective benefits packages, emphasizing transparency and fairness in direct reimbursement compensation methods.
The shared vision of RiskManagers.us and clients who retain our services is to establish and maintain a comprehensive employee health and welfare plan, identify cost areas that may be improved without cost shifting to any significant degree, and ensure a superior and sustained partnership with a claim administrator responsive to members needs on a level consistent with prudent business practices.
Plan costs, in all areas including fixed expenses and claims are open for review on a continuing basis. Cost effective plan administration and equitable benefit payment to providers are paramount to fulfilling our mutual fiduciary duties. As we proactively monitor and manage an entire benefit program we are open to any suggestions members may make or the dynamic health benefit market may warrant in order to accomplish these goals.
Duty of loyalty to our clients, transparency and accountability are essential to the foundation of our services. To that end, we expect our clients to realize a substantial savings based upon the services that we will deliver.
2021 RiskManagers.us All Rights Reserved

